In cases of diffuse goitre, there will be follicular cell hyperplasia. The majority of cystic thyroid lesions are hyperplastic nodules that have undergone extensive liquefactive degeneration by the time they are detected. 11 Pathologically, these are often known as hyperplastic and colloid nodules, sometimes they may also be described as adenomatous. The most important factor of colloid goitre appearance is a reduction in TSH stimulation for a prolonged period of time. 9 There is no correlation between race and the prevalence of goitre. 8,9 The peak age for the onset of goitre is 35–50 years, and the ratio of women to men affected by goitre is 3:1. 7 According to some studies, iodine deficiency is associated with a 5–10% prevalence of goitre. 4 It has also been suggested that thyroid function control factors, such as C cells, can alter iodine levels, leading to goitre. There is evidence that iodine supplementation can decrease the incidence of goitre in these people however, some cases of longstanding endemic goitres do not always regress with iodine supplementation. 5,6 An iodine-deficient diet is also known to lead to colloid nodular goitres. 2,4 A number of possible factors leading to colloidal goitre include foods that block the hormonal synthesis, mutations in thyroid-stimulating hormone (TSH) receptors, globulin stimulation of thyroid development, growth hormone, insulin-like growth factor 1 (IGF-1) and genetic factors. There are many mechanisms and aetiologies that cause colloid goitre ( Table 2). This article provides an overview of the aetiology, epidemiology, pathophysiology, histopathology, clinical manifestations and ultrasound features of colloid goitres, as well as differential diagnosis and management. In addition, the search was expanded to include terms such as ‘thyroid nodule’, ‘thyroid pathology’, ‘treatment of thyroid pathology’, ‘thyroid ultrasound’, ‘thyroid malignancy’, ‘thyroid cytopathology’, ‘thyroid evaluation’ and ‘thyroid nodule management’. Search terms included: ‘colloid goitre’, ‘diffuse hyperplasia’, ‘nodular thyroid’, ‘nontoxic goitre’, ‘endemic goitre’, ‘simple goitre’, ‘nontoxic uninodular goitre’, ‘nontoxic multinodular goitre’, ‘nodular hyperplasia’, and ‘colloid nodule’. We conducted searches on the PubMed database for articles published between September 1967 and August 2020 to provide a summary of key issues and updates related to colloid goitre. 
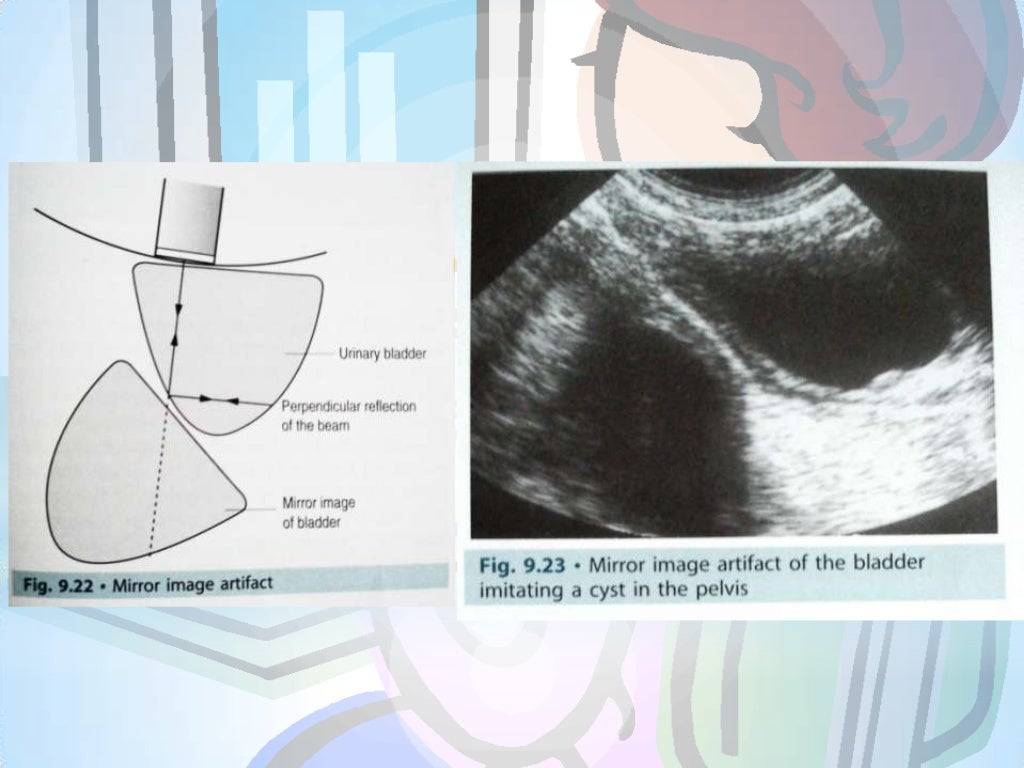
They are benign lesions however, on the ultrasound image, they can mimic malignant lesions. 1 Colloid goitre is also known as endemic goitre, simple goitre, nontoxic uninodular goitre, nontoxic multinodular goitre or nodular hyperplasia. Colloid goitre has been classified as nontoxic goitre according to the updated International Classification of Diseases ( Table 1). This is a common pathology, frequently found in clinical practice during a physical or ultrasound examination. KeywordsĬolloid, diffuse hyperplasia, nodular thyroid, nontoxic goitre, ultrasound Article:Ĭolloid goitre is defined as thyroid enlargement without accompanying disturbance in thyroid function. This review discusses the epidemiology, pathophysiology, clinical manifestations, ultrasound features and management of colloid goitres. However, some cases of colloid goitre do not show a comet-tail sign and sometimes these artefacts need to be distinguished from microcalcifications in malignant lesions. An important feature of colloid goitre is the contained colloid material inside and the comet-tail artefacts, which show up on ultrasound. 
Colloid goitres are a common, benign lesion of the thyroid gland, that involve a diffuse or nodular pattern. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
